Tracking
Most food diaries capture too much or too little. Here's exactly what to log for IBS and food sensitivity tracking — and what's just noise that wastes your time.
2 February 2026

I've seen a lot of food diaries. Some are beautiful, obsessively detailed records that take 20 minutes per meal to fill in. Others are scrappy notes that say things like "lunch - sandwich?" with a question mark. Neither is particularly useful.
The goal of a food diary isn't to document everything you eat. It's to generate enough structured data to identify patterns between what you consume and how you feel. That requires capturing the right things — consistently — not everything.
Here's what actually matters, what's useful in some situations, and what you can safely ignore.
"Chicken salad" is useless. "Chicken breast, romaine lettuce, cherry tomatoes, cucumber, olive oil, lemon juice, garlic" is useful.
Why does this matter? Because your trigger might be garlic, not chicken. If you record meal names, you'll never find it.
For home cooking, list the main ingredients. For restaurant meals, note the key components and any sauces, dressings, or seasonings. For packaged foods, note the brand and product name — you can check the ingredients later if needed.
You don't need to list every trace ingredient. Focus on anything present in a meaningful quantity. If you ate a bolognese, you don't need to list "1/4 tsp black pepper" — but you do need to list "onion" and "garlic" even if they were cooked into the sauce.
Log when you ate, not just what. Food sensitivities and IBS reactions are frequently delayed — sometimes by 12–24 hours. Without timestamps, you can't connect a Tuesday bloating episode to Monday's dinner.
When symptoms appear, note:
Severity ratings feel subjective, but over weeks of data they become surprisingly informative. A consistent "4/5 bloating" after certain meals that never appears after others is a meaningful signal.
This is the one people skip because it feels awkward to write down. Don't skip it.
Log frequency and use the Bristol Stool Scale (1–7) for consistency. Type 6–7 is loose/watery. Type 1–2 is hard/lumpy. Type 3–4 is the healthy range. Knowing your pattern on bad days versus good days helps identify what "better" actually looks like.
A single daily number from 1 to 5 is enough. Stress is a physiological trigger for IBS — it changes gut motility, lowers pain thresholds, and alters gut permeability. If you're not tracking it, you're missing a major variable.
Sleep deprivation worsens gut symptoms. If you suspect sleep is a factor, add a quick note (good/okay/poor or a 1–5 rating). You don't need to track it forever — just enough to see if there's a pattern.
For women, hormonal fluctuations have real effects on gut motility and sensitivity. If your symptoms seem to worsen at certain points in your cycle, tracking cycle day (or just phase: follicular/ovulation/luteal/menstruation) alongside symptoms can be revealing.
Heavy exercise can trigger symptoms in some people with IBS. Gentle exercise often helps. If you suspect this is a variable, note if you exercised and what type.
Especially if you're starting something new. Some medications and supplements affect gut function significantly (iron supplements, magnesium, NSAIDs).
What you track in matters less than whether you track consistently. But some formats make consistency much easier:
Structured templates beat blank notebooks. A template means you never have to think "what should I log here?" — you just fill in the fields. Cognitive friction is the enemy of consistent tracking.
Digital over paper for most people, because you always have your phone. But paper works if you genuinely prefer it — the key is having it accessible when you need it.
Log immediately after eating, not at the end of the day. "What did I have for lunch?" is much harder to answer at 10pm than it is at 1:30pm when you've just finished.
Retrospective recall of food is surprisingly unreliable. Studies show that when people log food from memory at the end of the day, they miss around 20% of what they actually ate. For IBS tracking specifically, the missing 20% might be exactly where your trigger is hiding.
After 3–4 weeks, you have something to work with. The next step is analysis:
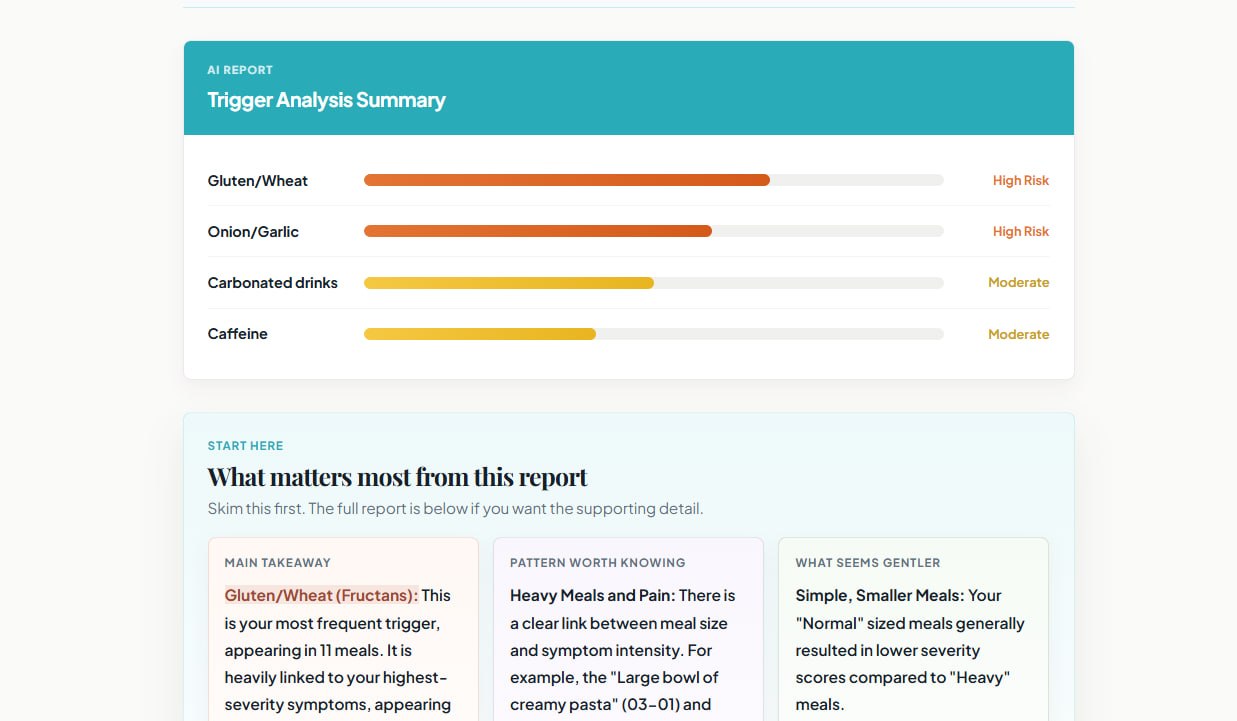
Manual analysis works but is time-consuming. This is where AI assistance becomes genuinely valuable — feeding your tracking data into an AI analysis tool can surface correlations across dozens of variables that would take hours to spot manually.
The IBS & Food Sensitivity Tracker makes logging simple — then uses AI to find patterns you'd miss on your own.
Get the Tracker →Track ingredients (not meal names), time of eating, symptom type/severity/timing, bowel movements, and a daily stress rating. That's the essential minimum. Skip calories, exact weights, and anything else that adds friction without adding signal. Log immediately after eating, use a structured format, and plan to analyse after 3–4 weeks of consistent data.
A simple, low-pressure way to start noticing patterns between what you eat, how your gut feels, and what might actually be triggering symptoms - before you commit to the full tracker.
Free — delivered straight to your inbox
🔒 No spam, we promise. Unsubscribe any time.